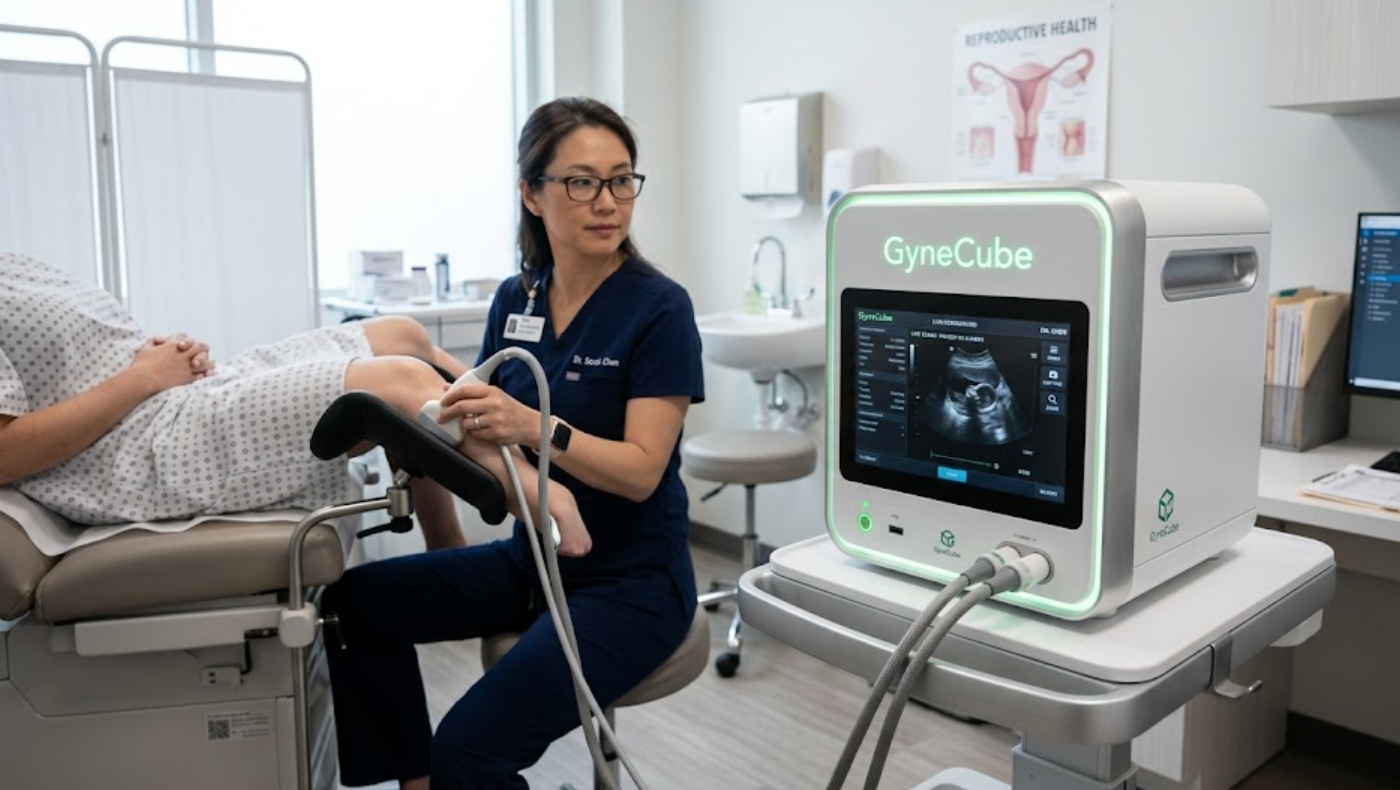
GyneCube is an advanced automated molecular diagnostic system designed to detect high-risk human papillomavirus (HPV), the primary cause of cervical cancer. Developed to streamline laboratory workflows, it uses PCR-based technology to identify HPV DNA with high accuracy and minimal manual involvement. The system integrates multiple steps—sample preparation, nucleic acid extraction, amplification, and detection—into a single automated process. This not only reduces human error but also ensures consistent and reliable results across large batches of samples. With its ability to process multiple specimens simultaneously and deliver standardized outputs, GyneCube plays a crucial role in modernizing cervical cancer screening by making it faster, more scalable, and more efficient for healthcare providers.
The Importance of HPV Testing in Cervical Cancer Prevention
Human papillomavirus (HPV) is recognized as the leading cause of cervical cancer, with high-risk strains such as HPV 16 and 18 responsible for the majority of cases worldwide. Early detection of these high-risk infections is critical because HPV can remain asymptomatic for years before progressing into cancer. This is where HPV testing becomes a vital component of preventive healthcare. Unlike traditional cytology-based methods, HPV testing directly identifies the presence of viral DNA, allowing for earlier and more accurate detection of potential risks. By focusing on the root cause rather than visible cellular changes, healthcare providers can intervene sooner and significantly reduce the chances of cancer development.
The introduction of automated systems like GyneCube has further strengthened the effectiveness of HPV testing in cervical cancer prevention. With its ability to deliver precise and rapid results, it supports large-scale screening programs and ensures that more women are tested efficiently. This is particularly important in regions where access to skilled cytologists is limited, as automation helps maintain consistent diagnostic quality. By improving detection rates and enabling timely follow-up care, GyneCube contributes to a proactive approach in reducing cervical cancer incidence and mortality, aligning with global health goals aimed at eliminating this preventable disease.
Key Features That Make GyneCube Stand Out
GyneCube distinguishes itself in the field of cervical cancer screening through its high level of automation, precision, and efficiency. One of its most notable features is its fully integrated workflow, which eliminates the need for multiple instruments and reduces manual handling, thereby minimizing errors and contamination risks. The system supports high-throughput testing, allowing laboratories to process numerous samples simultaneously without compromising accuracy. Additionally, its ability to deliver fast and standardized results enhances clinical decision-making and improves patient management. Another key advantage is its flexibility, as GyneCube can be adapted for various molecular assays beyond HPV testing, making it a versatile solution for modern diagnostic laboratories.
Clinical Accuracy and Performance: What Studies Show
The clinical reliability of GyneCube has been evaluated in multiple studies, with results consistently demonstrating high sensitivity and specificity for detecting high-risk HPV infections. These performance metrics are essential in screening programs, as they determine how effectively the system can identify true positive cases while minimizing false negatives. Research comparing GyneCube with other established HPV testing platforms has shown comparable, and in some cases favorable, outcomes, reinforcing its credibility as a dependable diagnostic tool. Such accuracy is particularly important in early detection, where identifying infections before they progress can significantly reduce cervical cancer risk.
In addition to accuracy, GyneCube has shown strong reproducibility across different laboratory settings, meaning results remain consistent regardless of where or by whom the test is conducted. This consistency is crucial for large-scale screening initiatives and national healthcare programs that rely on standardized testing protocols. The system’s automated nature further enhances performance by removing variability associated with manual procedures, ensuring uniform quality in every test run. As a result, GyneCube is increasingly recognized as a reliable solution that meets the clinical demands of modern cervical cancer screening.
Benefits of Automation in Cervical Cancer Screening
Automation has significantly improved the efficiency and reliability of cervical cancer screening, and systems like GyneCube are at the forefront of this transformation. By reducing manual intervention, automation minimizes human error, ensures consistent test quality, and accelerates turnaround times for results. This allows healthcare providers to screen more patients in less time, which is especially valuable in high-demand or resource-limited settings. Additionally, automated systems standardize workflows across laboratories, making large-scale screening programs more practical and effective while ultimately supporting earlier detection and better patient outcomes.
Real-World Applications and Case Studies
In real-world healthcare settings, GyneCube has been increasingly adopted in clinical laboratories and national screening programs focused on cervical cancer prevention. Its ability to process large volumes of samples efficiently makes it especially useful in population-based screening initiatives, where thousands of women may need to be tested within short timeframes. Hospitals and diagnostic centers using automated HPV testing systems report improved workflow organization, faster reporting times, and better allocation of laboratory resources. In many cases, GyneCube is integrated into existing molecular diagnostic platforms, allowing institutions to upgrade their screening capabilities without completely overhauling their infrastructure.
Case studies from screening programs in Europe and Asia have highlighted how automation improves participation outcomes and follow-up rates. For example, when high-risk HPV cases are identified more quickly and accurately, healthcare providers can ensure timely colposcopy referrals and early intervention. This reduces the likelihood of patients being lost to follow-up, a common issue in traditional screening systems. Overall, the real-world implementation of GyneCube demonstrates its practical value not only as a diagnostic tool but also as a system that strengthens the entire cervical cancer care pathway.
Challenges and Limitations of GyneCube
Despite its advanced automation and strong diagnostic performance, GyneCube is not without limitations. One of the primary challenges is the initial cost of installation and maintenance, which can be significant for smaller laboratories or healthcare facilities in low-resource regions. While the system reduces long-term labor costs, the upfront investment in equipment, reagents, and infrastructure may still be a barrier to widespread adoption. Additionally, like other molecular diagnostic platforms, it requires stable technical support and trained personnel for operation, troubleshooting, and quality control to ensure optimal performance.
The Future of HPV Screening with GyneCube
The future of cervical cancer prevention is increasingly moving toward fully automated, high-precision molecular screening, and GyneCube is positioned to play a meaningful role in that evolution. As healthcare systems continue to adopt HPV primary screening as a first-line strategy, demand for scalable and reliable diagnostic platforms is expected to grow. GyneCube’s automation capabilities align well with this shift, offering the potential for faster population-level screening and more efficient triage of high-risk patients. In the coming years, improvements in assay sensitivity, workflow integration, and digital reporting are likely to further enhance its role in laboratory medicine.
At the same time, integration with broader digital health ecosystems is expected to shape how systems like GyneCube are used. Future developments may include smarter data analytics, improved connectivity with electronic health records, and AI-assisted interpretation of results. These advancements could help healthcare providers identify trends earlier and optimize screening strategies at both individual and population levels. As global health initiatives push toward the elimination of cervical cancer, technologies like GyneCube will likely become increasingly central to achieving faster, more accurate, and more accessible screening worldwide.
Conclusion
GyneCube represents a significant step forward in the evolution of cervical cancer screening by combining molecular precision with full laboratory automation. Its ability to detect high-risk HPV efficiently and consistently makes it a valuable tool in modern preventive healthcare. By reducing manual workload, improving turnaround times, and supporting large-scale screening programs, GyneCube helps strengthen early detection strategies that are essential for reducing cervical cancer incidence and mortality worldwide. While it is not a standalone diagnostic solution, its role within a broader clinical pathway is increasingly important as healthcare systems shift toward more proactive and technology-driven screening models.
FAQs
Q1: What is GyneCube used for?
It is used for automated detection of high-risk HPV infections linked to cervical cancer.
Q2: Is GyneCube a replacement for Pap smear tests?
No, it complements screening programs but does not fully replace cytology-based methods.
Q3: How accurate is GyneCube?
Studies show it has high sensitivity and specificity for detecting high-risk HPV strains.
Q4: Why is HPV testing important?
Because persistent high-risk HPV infection is the main cause of cervical cancer, early detection helps prevent disease progression.
For More Gossip’s and Information Visit Star Story Time